Adopting the WHO Antenatal Care SMART Guidelines to Indonesia
As countries embark on digitalizing the health sector to achieve universal health coverage, the World Health Organization (WHO) launched the SMART — Standards-based, Machine-readable, Adaptive, Requirements-based, and Testable — Guidelines approach to optimize the adoption of WHO guidelines through digital systems.
SMART Guidelines are a package of tools that include Digital Adaptation Kits (DAKs), which detail the generic health workflows, core data elements, and decision logic derived from WHO guidelines as a starting point for incorporation into digital systems. Additionally, SMART Guidelines include reference software modules derived from WHO guidelines
WHO ANC SMART Guidelines provide implementation resources and guidance supporting applying the WHO recommendations on antenatal care (ANC) for a positive pregnancy experience. The Implementation Guide is part of the WHO Smart Guidelines approach to support countries in the integration of WHO global data and health recommendations into digital systems accurately and consistently. This new approach to global health in the digital age begins with maternal health and the launch of the WHO Smart Antenatal Care Guidelines.

WHO SMART Guidelines components
Since the release of the WHO Antenatal Care Guideline Implementation Guide, Ona has been researching how we can adopt and apply it to the work we do with our partners in antenatal care health projects using the FHIR-based OpenSRP platform. Over the last year, we have been working in partnership with PATH and Digital Square to understand how the WHO’s global antenatal care digital adaptation kit can be specifically applied to manage antenatal care in the Indonesian context.
Building a Reference App for Team-based Antenatal Care
To better understand how to use these care guidelines in a real-life project, we worked closely with the Lombok, Indonesia-based Summit Institute of Development (SID) to develop simplified content for the Indonesian context. The Summit Institute of Development was a founding member of the OpenSRP digital health platform and has decades of experience delivering team-based healthcare and next-generation health program research. To accelerate our progress towards a usable application, we converted the WHO Antenatal Care Guideline Implementation Guide to an FHIR-based OpenSRP app, that we could load onto mobile devices and dynamically update as we iterated on the forms and patient care plans. This allowed us to deliver the ANC health workflow content and user interface configuration while staying within the FHIR specification. We reviewed the WHO antenatal care digital adaptation kit and made the required adaptations for the Indonesian context, including creating a data dictionary aligned with the antenatal care digital adaptation kit but specific to Indonesia.
In addition, we designed a health workflow scenario to formulate acceptance criteria to test each of the specified routine antenatal care contacts. Digital adaptation kit components include:
- Linked health interventions and recommendations
- Personas
- User scenarios
- Business processes and workflows
- Core data elements mapped to standard terminology codes (e.g., SNOMED, LOINC)
- Decision support
- Program indicators
- Functional and non-functional requirements
Each of these components includes data requirements that are either met or unmet, and a corresponding FHIR Questionnaire, either explicitly specified, or derivable from data that is assumed to exist. These Questionnaires are used as an interface for completing activities such as:
- Rapid assessment and management (RAM)
- Danger signs needing referral
- Confirm pregnancy
- First contact
- Quick check
- Profile
- Check symptoms and follow up
- Conduct physical exam
- Conduct laboratory tests and imaging
- Counselling, in-facility management and treatment
- Urgent referral
- Scheduling
- Self-care in the home or community
Key Learnings
Over an extensive period of research, development and implementation of the WHO antenatal care SMART Guidelines we were able to seamlessly integrate the implementation guide into the OpenSRP workflows and provide a starting point for further country-specific adaptation of the guidelines and management of the content collected through them. Additionally, the implementation guide provides a set of FHIR Measures and Clinical Quality Language (CQL) scripts used to generate indicators for the monitoring and evaluation of various performance metrics relevant to antenatal care.

The Summit Institute of Development digital health team assisting a midwife who is using the antenatal care app.
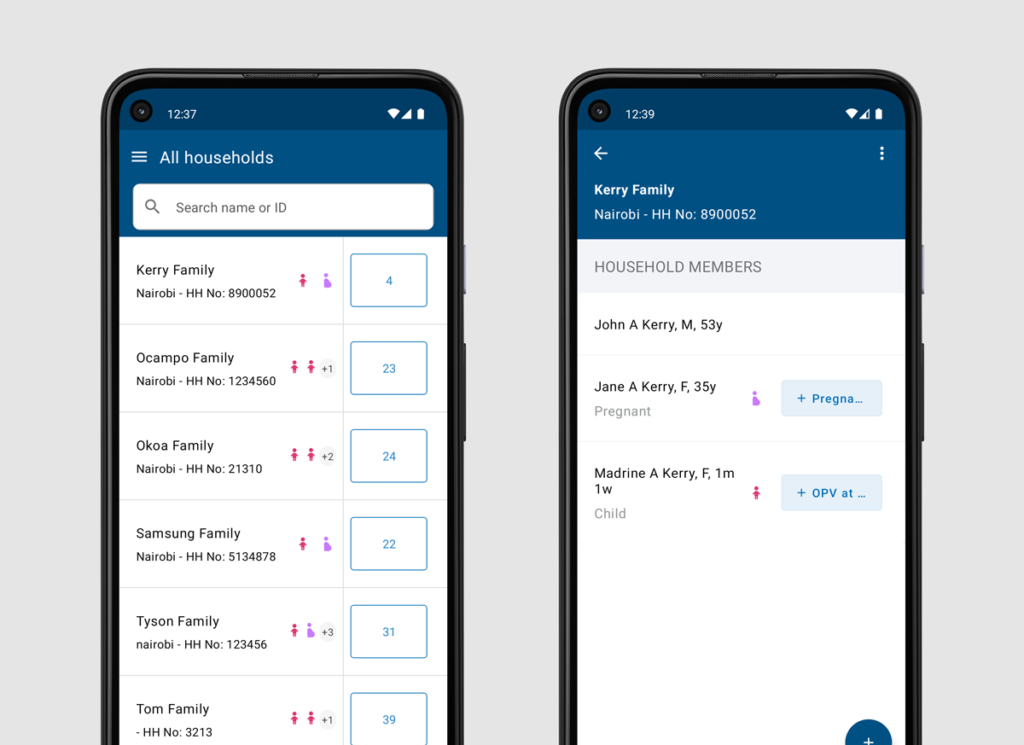
The family list and family view screens in the Indonesian adaptation of the WHO Smart Guidelines antenatal care implementation guide.
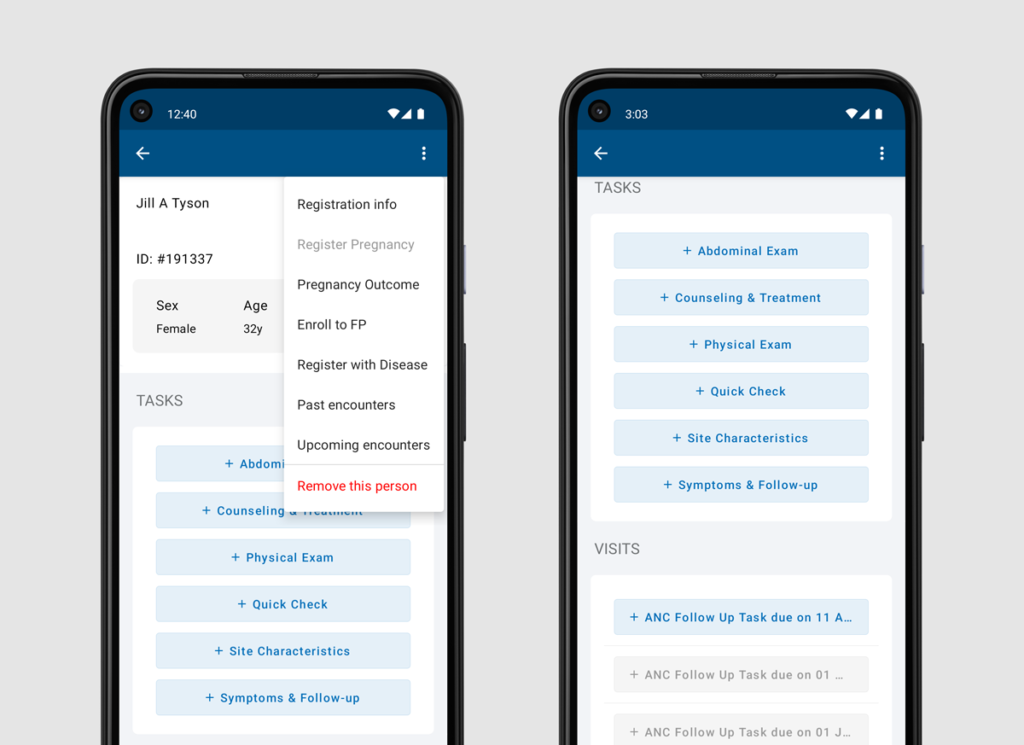
The patient profile with menu shown and patient task as well as visit list screens in the Indonesian adaptation of the WHO Smart Guidelines antenatal care implementation guide.
What worked
The antenatal care digital adaptation kit provides content on health care practices and delivery that prioritize person-centred health and well-being, not only the prevention of death and morbidity, by following a human rights-based approach. This guideline is relevant to all pregnant women and adolescent girls receiving antenatal care in any healthcare or community setting and their unborn fetuses and newborns. This is also supported via decision support provided via Clinical Quality Language (CQL) scripts embedded in various workflow content such as the various check in the FHIR Questionnaires and antenatal care FHIR PlanDefinitions.
The digital adaptation kit provides an example of how to sequence workflows to effectively provide care to the end users, while also providing a guide on how to train end users, i.e. how community health workers can best capture client information. This helps to avoid problems, such as having inconsistent data collection methods or lacking a consistent data format. This guideline covers recommendations in various areas including nutrition, maternal and fetal assessment, preventative measures, interventions for common physiological symptoms and interventions to improve antenatal care utilization and quality of care.
What did not work
In the process of converting the digital adaptation kit to work with a production-ready health platform, we experienced the following summarized issues that provide room for both further improvement as well as research and design to work towards their resolution:
Usage of In-line CQL Script
No clear mechanism can trigger in-line CQL is provided via text/cql-identifier. This may be a knowledge gap and may require knowledge sharing from the CQL community or CQL authors.
Usage of valuesets
It was unclear how an implementer connects to an appropriate valueset terminology server in order to sync the required drop-down options for the input spinners. This may be considered a knowledge gap and may require some knowledge sharing from the WHO Computable Guidelines Community.
Usage of ActivityDefinitions
ActivityDefinitions are supplied however we cannot execute the ActivityDefinition-apply operation because this is not provided in the Android FHIR SDK, and because the specification is not fully covered in the WHO Computable Guidelines Implementors Community calls and forums.
ANC Content bundled on the DAK
- There are no defined form data extraction processes for creating new resources, such as Patients, RelatedPerson, Encounters, Observations, Conditions, Flag, Groups etc.
- For the Encounters, Observations and Conditions there are limited references on which SNOMED or LOINC code to use to define the desired concepts in use and later mapped for indicator-based reporting purposes. A list of antenatal care indicators is defined (via measures and CQL scripts) but it is not clear what data is expected to be extracted to which resources upon form submission and how it maps to aggregations for indicator reporting.
- Unintuitive user experience for filling in the questionnaires as some are either too lengthy or contain questions that could be answered in other sections of the workflows and still accomplish the same purposes.
Conclusions and Future Work
Identifying the customization requirements of the antenatal care digital module through the digital adaptation kit provided an opportunity to strengthen the content within the country-customized module, as well as support other digital systems to align with the WHO clinical recommendations and digital health standards. Ona is continuing its collaboration with the Summit Institute of Development to adapt the digital adaptation kit to the specific country context.
Although we use antenatal care as an example to illustrate the adaptation of a specific healthcare module using the digital adaptation kit, the process of customizing SMART Guideline components will be relevant for any particular health domain area. This process demonstrated that it is critical to align any new digital tool with existing digital governance systems and to ensure local ownership. Collaboration and constant engagement from the project’s outset between the maternal program and ICT leads were critical to coordinate requirements for the adaptation of the WHO ANC digital module to the Indonesia-specific context.
As the SMART Guidelines, including the digital adaptation kits, are a new approach, it will be important to capacitate Ministries of Health and digital health implementers to ensure ownership of the adaptation processes from the outset. We would like to thank the team at PATH and Digital Square for their insightful advice and guidance throughout the course of this project.
If you are interested in learning more about this work or partnering with us to use digital health platforms and standards to reduce child mortality, we would love to hear from you, fhir@ona.io, on Twitter @onadata and LinkedIn.

